Leaky Gut: Understanding the Gut Lining
The term “leaky gut” is commonly used, but what does it actually describe?
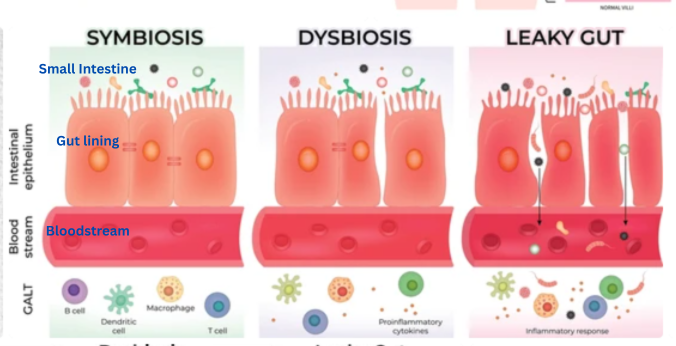
The image below illustrates three states of gut health: Symbiosis, Dysbiosis, and Leaky Gut.
Let’s walk through what you’re seeing.
Where This Happens
At the top of the image is the small intestine.
The pink cells form the gut lining — a protective layer that separates what remains inside the digestive tract from what enters the bloodstream.
Below that is the bloodstream, where nutrients are absorbed and transported throughout the body.
The gut lining is not passive.
It is a dynamic, selective barrier.
Symbiosis: A Balanced System
In the first panel:
Beneficial microbes are present in healthy balance.
The cells of the gut lining sit closely together.
Tight junctions regulate what passes through.
Nutrients enter the bloodstream appropriately.
The immune system remains calm.
This is the intended design.¹
Dysbiosis: Microbial Imbalance
In the second panel:
The balance of microbes shifts.
Harmful organisms increase.
Inflammatory signaling begins to rise.²
The gut lining may still appear structurally intact, but irritation is present.
Dysbiosis does not automatically mean leaky gut — but it can contribute to ongoing stress within the system.
Leaky Gut: Increased Intestinal Permeability
Notice in the third panel:
The spaces between the gut lining cells widen.
Larger particles pass into the bloodstream.
Immune cells activate.
Inflammatory response increases.
This widening of the junctions between cells is called **increased intestinal permeability.**¹
When partially digested food proteins, microbial fragments, or toxins enter circulation prematurely, the immune system recognizes them as foreign.³
Research has linked increased intestinal permeability with autoimmune conditions and other chronic inflammatory states in some individuals.²
Leaky gut is not a diagnosis.
It is a mechanism that may contribute to broader processes.
When Might This Be Relevant?
Increased intestinal permeability has been observed in association with certain immune-related conditions in some individuals, including:
Rheumatoid arthritis
Hashimoto’s thyroiditis
Psoriasis
Celiac disease
Inflammatory bowel conditions
This does not mean leaky gut causes these conditions.
It means the integrity of the gut lining may be one contributing factor worth understanding as part of a broader clinical picture.²⁴
If you are living with one of these diagnoses — or navigating persistent inflammatory symptoms — it may be appropriate to discuss gut health with your physician.
What Contributes to Permeability?
Increased intestinal permeability is rarely about one single food.
More often, it reflects that the system has been under strain.
That strain can come from:
Highly processed foods eaten regularly
Ongoing digestive irritation
A lack of dietary variety
The gut lining responds to the environment it lives in.
When that environment improves, it often becomes more resilient.
Three Simple Foods That Support Gut Health
You do not need a complicated protocol to begin supporting your gut lining.
Here are three widely available foods that can help:
1. Plain Yogurt (with live cultures)
Unsweetened yogurt contains beneficial bacteria that support microbial balance.²
Look for “live and active cultures” and avoid added sugars.
If dairy is not tolerated, choose an unsweetened plant-based version with live cultures.
2. Oats
Oats provide soluble fiber, which feeds beneficial gut bacteria.²
This process supports the production of short-chain fatty acids — compounds that help maintain the integrity of the gut lining.
Start with modest portions if digestion is sensitive.
3. Cooked Vegetables
Cooked vegetables such as carrots, zucchini, and spinach are often easier to digest than raw varieties.
They provide fiber, antioxidants, and phytonutrients that support the gut ecosystem.
Consistency matters more than complexity.
Questions to Bring to Your Physician
If you are managing inflammatory or autoimmune symptoms, you might consider asking:
Could gut inflammation be contributing in my case?
Should celiac disease be ruled out before removing gluten?³
Would dietary modification be appropriate?
Is further evaluation indicated?
These are collaborative conversations.
A Calm Approach
The goal is not perfection.
The goal is stability.
The gut lining functions best when:
The microbiome is diverse
Inflammation is regulated
Stress signaling is balanced
The immune system can tolerate what is harmless and respond appropriately to what is not⁴
Small, consistent changes can strengthen that boundary over time.
If You’d Like Support
If you’d like structured support exploring whether gut health may be relevant in your case — and how to approach it thoughtfully — you can schedule a discovery call here.
Education is the first step.
Implementation is the second.
Footnotes
Basics of Digestion Study Guide – Tight junctions and intestinal permeability Study Guide_ Basics of Digestion
Balancing the Microbiome Study Guide – Dysbiosis, permeability associations, fiber and microbiome support Study Guide_ Balancing the Micr…
Lukaczer, D. “Removing Foods that Contribute to Intestinal Permeability and Inflammation” – Immune activation and gluten testing considerations Removing Foods that Contribute …
Coaching for Immune Health Study Guide – Immune tolerance and gut-immune regulation Coaching for Immune Health. M4.…